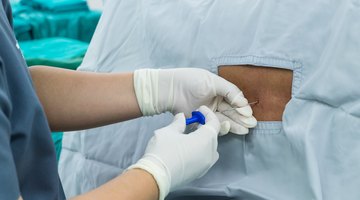
Side Effects of a Spinal Block for a C-Section
According to John S. McDonald, MD, chairman of the department of anesthesiology and professor of obstetrics and gynecology at UCLA Medical Center, spinal block has emerged as the preferred approach to Cesarean section anesthesia based on the finding of higher maternal mortality among patients who undergo general anesthesia.
Spinal blocks also offer other advantages over general anesthesia, such as allowing the mother to be awake during the birth of her child, reducing the child’s exposure to anesthetic drugs, decreasing the risk of maternal complications that do not result in death and, finally, providing a convenient way to manage postoperative pain. As with any procedure, spinal block sometimes produces side effects.
Mild Respiratory and Circulatory Depression
In some cases, the medication used to induce spinal anesthesia travels higher than intended within the spinal cord, a condition doctors refer to as high neural blockade or high spinal block. High neural blockade occurs most often in obese or short women, and in women who are unusually sensitive to anesthesia. The result is mild respiratory and circulatory depression.
Patients typically describe mild shortness of breath and numbness or weakness in the arms, shoulders and trunk, followed by nausea, with or without vomiting. High spinal block may be frightening, but it is not life threatening. Treatment consists of reassurance, supplemental oxygen and intravenous drugs that rapidly correct heart rate and blood pressure.
Back Ache

Epidural Side Effects and Risks
Learn More
Back aches related to spinal anesthesia may result from tissue trauma during insertion of the spinal needle through the layers of skin, fat, muscles and ligaments. It’s unclear whether spinal anesthesia specifically causes back ache, because, according to Dr. Wayne Kleinman, director of Obstetrical Anesthesia at Encino-Tarzana Regional Medical Center in Tarzana, California, in the 2006 edition of “Clinical Anesthesia,” 25-30 percent of patients who receive general anesthesia--which does not involve insertion of a needle through the tissues of the back--also report back aches, as do many obstetric patients who undergo neither Cesarean section nor anesthesia.
Patients usually describe pain as mild soreness or aching.
In rare cases, back ache can signal the presence of more serious problems such as a localized collection of blood, known as a hematoma, or a localized collection of pus, known as an abscess.
Once hematoma and abscess have been ruled out, patients can manage pain with warm or cold compresses or acetaminophen. Most cases resolve within a few weeks.
Headache
Puncture headaches result from leaks in the cerebrospinal fluid related to needle puncture for spinal anesthesia. While they are not serious, they are uncomfortable. Patients typically describe pain around the forehead, behind the eyes or at the base of the skull, sometimes extending down to the neck. Pain may be throbbing and episodic, or constant and unremitting. In some case, headache also produces sensitivity to light and nausea.
Puncture headaches can be distinguished by their association with position—pain usually improves when the patient lays flat, only to resume with sitting or standing.
Spinal headaches usually appear 12 to 72 hours after a Cesarean section, although they sometimes begin immediately. With treatment, most resolve within a few hours.
Related Articles
- “Clinical Anesthesia;” G.E. Morgan et al.; 2006
- “Williams’ Obstetrics;” F.G. Cunningham et al.; 2010
- “Current Diagnosis and Treatment: Obstetrics and Gynecology, 10th edition;” A.H. DeCherney and L. Nathan (eds.); 2007