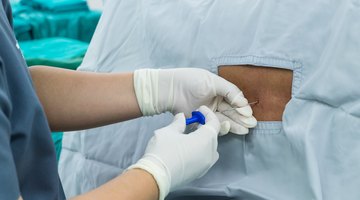
Epidural Side Effects and Risks
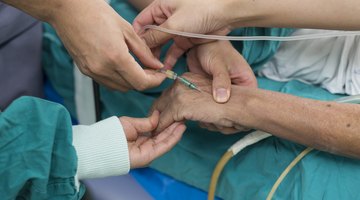
The purpose of an epidural injection is pain relief for herniated discs and labor pains. Local anesthetics, commonly referred to as numbing medications, and anti-inflammatory steroids placed into the epidural space during the injection decrease inflammation and swelling around the nerve roots causing the back pain, according to the Pain Management Center in Paducah Kentucky. Disc protrusions in the spine can compress on the nerves exiting from the spinal cord through the epidural space, causing pain. The space outside the dura, also known as the covering of the spinal cord, is the epidural space and covers the entire length of the spinal cord. When nerves from the epidural space are irritated or compressed, pain can radiate to the back, neck and legs. The injection placement depends on which nerve is affected. Although side effects do not occur often, there are a few signs to watch for following an epidural.
Headache
A postdural puncture headache, also called spinal headache, occurs when cerebrospinal fluid leaks from the puncture wound left by the needle penetration in the dura and can last for weeks. Spinal headaches result in 10 to 40 percent of all epidurals performed, according to “Understanding Medical Surgical Nursing” by Linda Williams and Paula Hopper. Lying flat and forcing fluids may help relieve pain, but if the headache continues a blood patch treatment may be necessary to stop the CFS leakage. Symptoms of a spinal headache can include persistent headache and photophobia, also called double vision.
Nerve Damage

Common Side Effects on Legs After an Epidural
Learn More
Whenever a needle passes near nerves and the spinal cord, nerve damage is a possible risk. If the injection needle touches the nerves or spinal cord, there are neurological signs, such as a sharp, shooting pain. Nerve damage caused by an epidural is very rare, according to the Mayfield Clinic, and any muscle weakness or numbness usually subsides within eight hours after the injection.
Infection
As with all procedures, infection is a possible risk with epidural steroid injections, but only results in about 2 percent of injections, according to Bigbackpain.com. Diabetics and other people with compromised immune systems are more susceptible to infection. Skin infections can pass into the epidural space and spread throughout and show symptoms of redness, warmth, drainage and pain at the injection site. Physicians typically prescribe antibiotics for this.
Decreased Bone Density
Headache After C-Section
Learn More
A decrease in bone density can occur with epidurals for back and neck pain, according to the Mayo Clinic. Corticosteroids, a natural hormone found in the body, given in the epidural will increase the natural body level and can affect bone cells, making bones at higher risk for fracture.
Other Steroid Side Effects and Risks
Herniated disc pain can worsen or remain the same after the epidural injection, as well as cause other secondary problems, such as:
- an allergic reaction to the medication
- epidural hematoma
- spinal-cord infarction
- puncturing an artery
- drop in blood pressure
- increased blood sugar levels in diabetics
- according to the Mayfield Clinic
Related Articles
- “Understanding Medical Surgical Nursing”; by Linda Williams and Paula Hopper; 2003
- The Mayo Clinic: Back Pain
- Mayfield Clinic: Epidural Steroid Injections
- US National Library of Medicine