How to Have a Successful Pregnancy With Low HCG
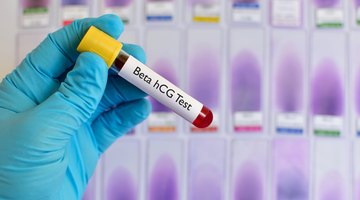
Human chorionic gonadotropin, also known as hCG, is the hormone measured by urine and blood pregnancy tests.
When you get pregnant, hCG is produced by tissue that will become the placenta. The production of hCG signals the corpus luteum, the remnant of the follicle that grew in the ovary, to keep producing progesterone, a hormone that prepares the uterine lining so that an embryo can grow.
When the placenta takes over progesterone production around the tenth week of pregnancy, hCG levels remain stable for the rest of the pregnancy. No action on your part will change your hCG levels.
Review your hCG levels with your medical provider. Your initial hCG level is not as important as the fact that the numbers should rise appropriately. Low hCG levels are normal at the start of pregnancy, but should double every 48 to 72 hours for the first seven to eight weeks of pregnancy. At the time of your first missed period, your hCG level usually ranges from 5 to 50 mIU/mL, with an average of 21 mIU/mL. By 11 days after conception, 98 percent of women have detectable hCG levels, according to Lawrence S. Neinstein, editor of “Adolescent Health Care: A Practical Guide.”
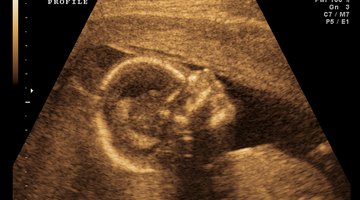
Track your hCG levels for the first two to three weeks of pregnancy. If you’ve undergone fertility procedures such as in vitro fertilization, your clinic may monitor your hCG levels for the first three weeks, until you have an ultrasound that shows a beating heart. By the time your hCG levels reach 3,600 mIU/mL, a transabdominal ultrasound should show fetal development in the uterus. With transvaginal ultrasound, fetal development should appear in the uterus when the hCG level reaches 2,000 mIU/mL, according to the American Pregnancy Association.
Watch for signs of problems if your hCG is not doubling appropriately in early pregnancy. While late implantation can account for an initial hCG level that’s lower than the norm, hCG levels that don’t rise appropriately could indicate an early fetal demise or an ectopic pregnancy, one that implants outside the uterus, usually in one of the fallopian tubes. Notify your doctor immediately if you have vaginal bleeding or abdominal pain, lightheadedness or dizziness, or if you pass out.
Realize that hCG levels will no longer double every two to three days after the seventh or eighth week of pregnancy. At this point, the placenta begins to produce more progesterone, and the role of the corpus luteum fades as it begins to disintegrate. Normal hCG levels after week eight range from 7,650 to 229,000 mIU/ml, the American Pregnancy Association reports. Levels will remain static and then slowly rise after week 22 until delivery, according to Neinstein.
Look at the fetal ultrasound, not the hCG numbers. If your baby is growing normally on ultrasound, the hCG levels are not important. Once the fetus develops a heartbeat at six to seven weeks of pregnancy, the chances that the pregnancy will continue are between 70 and 90 percent, according to the American Pregnancy Association.
Tips
If you ovulate later than expected during a given month, your initial hCG levels at the time you expect your period will be lower than normal. If the embryo implanted a day or two later than expected, initial hCG levels may also be low.