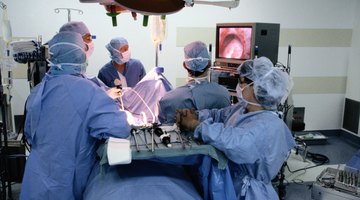
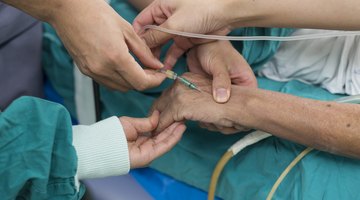
Albuterol with Infants
Albuterol is used with infants for the treatment of respiratory difficulties associated with certain illnesses. In some situations, the airway muscles of a baby tighten and spasm, reducing the ability to bring in oxygen. A baby may need to use the muscles of the abdomen or neck to attempt to get more air, or she may make wheezing or grunting sounds. Albuterol is a bronchodilator that works to relax the muscles of the airway to restore calm, natural breathing.
RSV
Respiratory syncytial virus is a contagious illness that most commonly affects children under the age of four. Babies who have RSV develop symptoms of a runny nose, cough and wheezing. According to the Cleveland Clinic, over 80,000 children are hospitalized for RSV complications each year. Albuterol may be used to treat acute wheezing in a baby with RSV, loosening the air passages to restore effective breathing.
Asthma
Complications of Aspiration During Surgery
Learn More
Asthma occurs when the lungs constrict as a response to an outside stimulus. Asthma is a chronic condition of stable breathing punctuated by attacks of wheezing, coughing and breathing difficulty. Albuterol may be used to treat asthma symptoms in babies as a type of rescue medication, meaning it is administered during the attack to emergently restore relaxed breathing.
BPD
Infants who are born prematurely may need supplemental oxygen after birth in the form of ventilation. Because a premature infant’s lungs contain very fragile tissue, prolonged ventilator use can lead to scarring and decreased elasticity, a condition known as bronchopulmonary dyplasia. Infants with BPD may have difficulty breathing and may have reduced stamina for activities. While there is no cure for BPD, regular treatments with albuterol may lessen some symptoms by relaxing the stiff lung tissue. Most infants eventually outgrow BPD and have few long-term effects.
Administration

Infant Reflux & Wheezing
Learn More
Albuterol is frequently administered to babies in the form of a nebulizer. Although albuterol may also be administered using an inhaler, this route is reserved for older children who can coordinate their breathing. Albuterol is dispensed in liquid form, frequently in pre-measured doses. Each dose is placed within a cup on the nebulizer and the machine is started. The machine changes the albuterol into a vapor that can be inhaled by a baby. The vapor is administered through a mask that may be placed on or near the baby’s face for treatment.
Side Effects
Babies who are given albuterol treatments may have side effects associated with the medication. Common side effects of albuterol include:
- an increased heart rate or racing pulse
- sweating
- fine tremors or nervousness
- vomiting
- diarrhea
- sleeplessness